Have you ever wondered what is actually in poo? Had it ever occurred to you that every persons’ poo is different and that its composition can actually tell us a lot about a persons’ diet and potential diseases that they could develop in the future? Microbiology lecturer, Dr Martin Goldberg explores new and powerful technology, that enables us to ask and answer questions that we never dreamed of being able to make until a few years ago about the human microbiome.
What is poo?
The majority of the biomass of poo is made of bacteria. However, it also contains left-overs from the food we eat, that our bodies cannot metabolise such as plant fibre.
Why does poo smell so bad?
The bacteria in our intestines play a critical role in helping us to digest and break-down the food we eat. As they break-down the food, they release a cocktail of unpleasant-smelling waste products such as amines, sulphides and mercaptans.
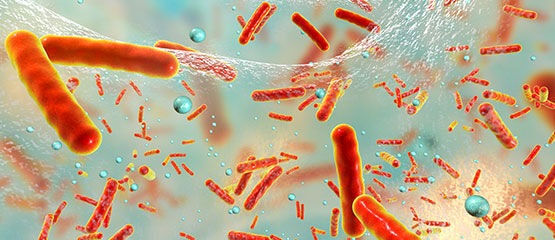
The human microbiome
You may have heard of the human microbiome in the news, on the Internet or in debates. The microbiome is the word we use to describe the collection of microbes that live inside us and on our bodies.
We now know that every persons’ microbiome is unique, just like our fingerprints - which we have only recently been able to learn thanks to the advent of Next-Generation DNA sequencing (NGS). Until the advent of NGS, we had not realised how many of the microorganisms living in our intestines had never been discovered before because nobody had been able to grow them in the lab. Thanks to NGS, we can find out about all the microorganisms living in and on our bodies in a matter of hours!
Our microbiomes – why are they so important?
During pregnancy, the baby is in a sterile environment. However, during birth, as the baby travels through the vagina, it becomes “inoculated” with Mum’s bacteria that live in the vaginal canal. Many of these bacteria, known as Lactic Acid Bacteria (LAB), are known to play crucial roles in the initial colonisation of the baby’s gastrointestinal tract. The LABs are important in “programming” baby’s immature immune system, teaching it how to respond to the many bacteria that eventually colonise the intestines.
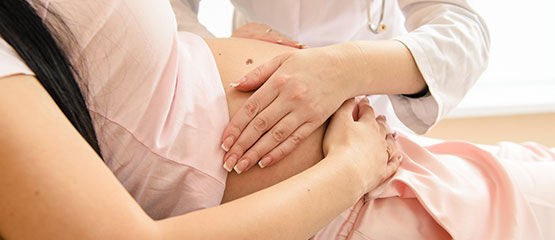
Babies born by Caesarean section may eventually become colonised by LABs, especially if they are breast-fed but it is also likely that they will develop very different gut microbiomes and this can sometimes have long-term consequences for the health of a person such as the development of Irritable Bowel Disease, Crohn's Disease, Necrotising Enterocolitis, Type II diabetes etc. Some researchers have been experimenting by taking the vaginal secretions from Mum and smearing them over her new-born baby to deliberately colonise the infant with “Good” bacteria.
Thanks to NGS, we have been able to correlate the presence and absence of several groups of bacteria with a number of serious, chronic diseases. We now know that the microbiome can affect:
- Development of Type II diabetes
- IBS
- Crone’s disease
- Bowel cancer
- Severity of symptoms in Autistic-spectrum disorder individuals
- Neurodegenerative conditions such as Parkinson’s Disease
What determines which bacteria live in our intestines? Can we change our microbiomes?
A number of factors are important in determining the composition of our microbiomes such as
1) Diet
2) Genetics of the individual
3) Early colonisation during birth / post-partum

We now know that the typical Western diet is not good for encouraging the growth of the “Good” bacteria. A good diet should contain plenty of fibre and plant matter such as fruit and vegetables and fish. The typical Western diet is rich in refined ingredients such as sugars, fats, salt and protein and this encourages the growth of very different microbiomes to those seen in people living on relatively unrefined diets eg in the Far East, Africa etc.
Poo as a cure for life-threatening diseases
People who have been to hospital for major surgery, e.g. to the bowel, will be given powerful antibiotics which eliminate virtually all the bacteria in our intestines. This allows antibiotic-resistant bacteria such as Clostridium difficile (often known as C. diff) to become established, particularly in elderly patients, which causes a life-threatening infection called pseudomembranous colitis, that is extremely difficult to cure.
Treatment with antibiotics may temporarily alleviate symptoms but they often return once the antibiotic course has finished. Patients suffer from chronic diarrhoea and abdominal pain and the intestine eventually becomes non-functional.
More and more hospitals are now turning to a very cheap and low-tech cure for C. diff patients which involves taking poo from healthy people such as relatives. The poo is put into a blender with a buffer solution, the unpleasant parts are removed and the bacteria introduced into the intestines of the patient through a tube. This faecal transplantation is proving to be a highly effective cure for C. diff patients.
The microbiome and bowel cancer
There is increasing evidence that development of bowel cancer can be triggered by our microbiomes. NGS has shown that some types of bacteria are associated with development of neoplasias and this is again due to diet.
Diet encourages colonisation of the intestine with some types of bacteria that produce waste products such as para-cresol that causes inflammation of the intestine which may eventually promote cancer. In mice, treatment with antibiotics can actually reverse early cancerous changes if caught in time!
The microbiome, diabetes and obesity
There is mounting evidence that as diet encourages the growth and colonisation of the intestines with “bad” bacteria which, as mentioned earlier, encourage people to eat more fast-foods, these bacteria cause inflammatory changes in the intestine, resulting in poor regulation of nutrient flow into the bloodstream. People who show increasing insulin resistance, meaning that their ability to regulate blood sugar levels becomes more difficult, eventually leading to diabetes.

Some patients who have changed their diets to eliminate fast-foods and replaced with diets rich in fruit, vegetables, fish and fresh meat, insulin sensitivity is restored, body mass index decreases and other health indicators show dramatic improvements.
Scientists are so confident about their findings that by taking poo samples and identifying the bacteria in a baby’s intestines, they can predict which ones will become obese by the age of 2!
What can we conclude?
Our microbiomes are very complex and sensitive to a number of factors but diet plays a pivotal role. Western lifestyles encourage the colonisation of our intestines with undesirable microorganisms that can have a number of consequences on our health and wellbeing. By taking more care of our microbiomes, we'll see a big improvement in many different facets of our lives.
